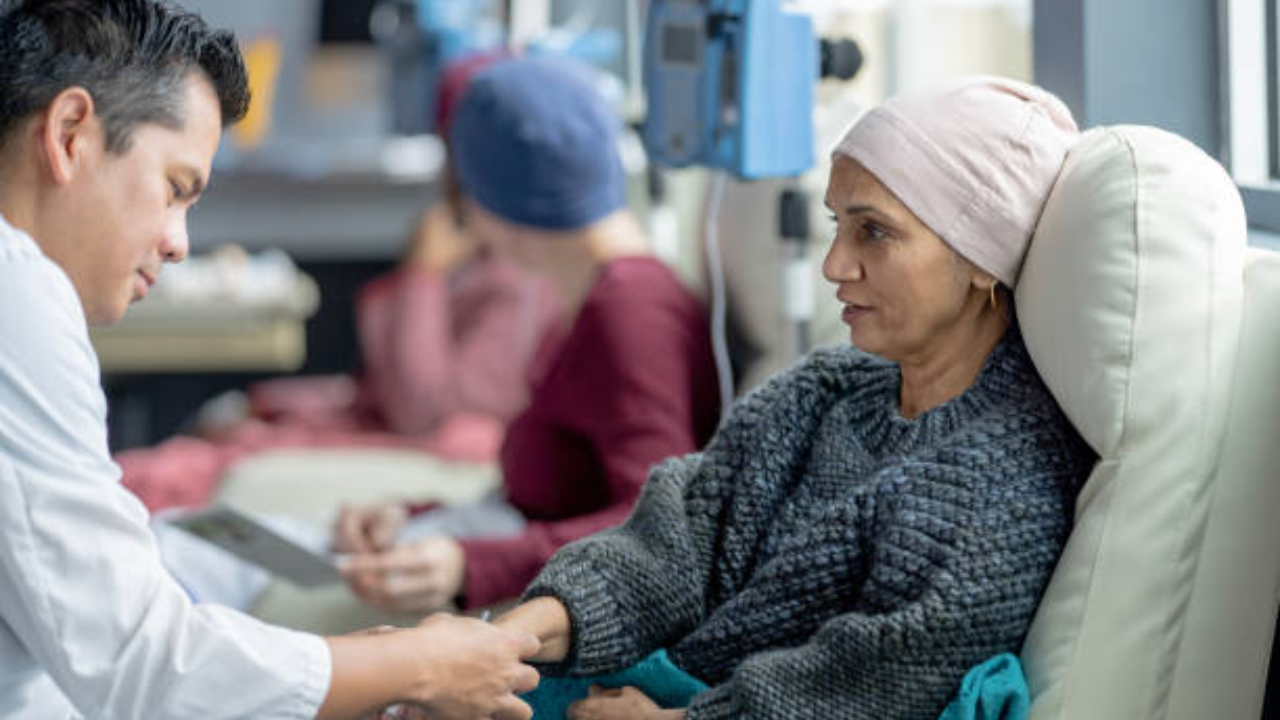
When people talk about cancer treatment, one word almost always comes up first: chemotherapy. Even if someone doesn’t know much about cancer, they have probably heard stories about chemo, hair loss, long hospital visits, nausea, and the idea of “strong medicines” fighting the disease.
Chemotherapy has been around for decades and has helped millions of people live longer, better lives. What it does? It uses powerful drugs to kill cancer cells or stop them from growing and spreading. Chemo is designed to target the fast growing cancerous cells.
However, cancer treatment isn’t one-size-fits-all
A lot of people also believe that chemotherapy is the only treatment for cancer, and that once someone is diagnosed, chemo automatically follows. This idea is so common that when someone hears the word “cancer,” the next thought is often, “they will have to do chemo,” no questions asked.
Watch
Breast Cancer: Early signs of the disease one must never ignore
Not every cancer needs chemotherapy, and not every patient is treated the same way. But because chemo has been the most visible and talked-about option for so long, many people assume it’s unavoidable.
Watch
Study: Artificial intelligence detects effectiveness of breast cancer chemotherapy
Breaking this myth is important.
Gurugram based Dr. Rohan Khandelwal, who is also the Head of Breast Centre, CK Birla Hospital, told TOI Health, the moment a patient is diagnosed with breast cancer, one of the first things on their mind is whether they will have to undergo chemotherapy.
Every patient who walks in is well aware of the significant side effects of chemotherapy and the impact it can have on an individual's overall quality of life. Many patients believe that chemotherapy is a must for everyone, irrespective of the stage of the cancer.
“The good news is that with advances in medicine, doctors are now rethinking chemotherapy for early-stage breast cancer patients,” says Dr Khandelwal.
Dr Khandelwal says understanding the stage of the cancer is very important to decide if chemotherapy is required or not.
“If it is at a later stage with an aggressive biology tumor, then we tend to do chemotherapy first and then surgery. In case of patients at an early stage and a favourable biology tumor, chemotherapy might be avoided. There are also a subset of patients where surgery is done first because it is operable, and the patient has a less aggressive tumor biology. After reviewing the post-surgery results, we determine whether chemotherapy or radiotherapy would be beneficial,” he explains.
“There are long-term trials that have been done, and our focus when considering chemotherapy or any other therapy for a cancer patient is disease-free survival and overall survival. As long as those figures are increasing without any substantial side effects of therapy, then we consider giving therapy to the patient. If the patient is going to substantially benefit from chemotherapy, then they are a candidate for it. If they don't have an absolute benefit from it, then there is no strong reason for giving them the side effects of chemo,” he says.
De-escalation of chemotherapy and why that is the way forward
Dr Khandelwal shares the case of a 52-year-old early-stage patient who suffered a sudden spike in hypertension and even a minor stroke during the usual post-surgery recovery period. She qualified for one of the molecular tests, which indicated a low-risk tumour, and she was safely able to avoid chemotherapy.
“The treatment is more biology driven, and oncologists are now trying to personalize it to the patients. There are tests for a specific subset which is early-stage breast cancer and hormone-positive (good biology tumors). In such patients, molecular tests can be done, and if these tests indicate a low-risk tumour and there’s low risk of recurrence, we can avoid chemotherapy in such patients,” he explains.
Any patient would be happy when you tell them they do not need chemo. Chemotherapy is the most dreaded part of cancer. With advances in medicine, many early-stage breast cancer patients now have the option to determine whether they will truly benefit from chemotherapy, the doctor said.
Any therapy comes with its own baggage of side effects, and in chemotherapy, there is hair loss, which is a major physical and emotional issue for women. Although it is reversible and hair does come back, for that period it is quite traumatising for the patient, and there can also be certain side effects of chemotherapy which can be long lasting as well. So, if chemotherapy is not adding any benefit to that subset of patients, then why should we subject them to unnecessary side effects, which in turn would mean better quality of life for the patient as well, says the doctor. Wherever de-escalation can be done, as long as it is backed by scientific evidence, it is definitely good for the patient, he concludes.